Testing, Testing, Not enough Testing
in Ars TechnicaIn response to:
America’s COVID-19 testing has stalled, and that’s a big problem
We'll need a lot more testing capacity to get the coronavirus under control.
Timothy B. Lee - 4/2/2020, 5:09 PM
One of America's biggest fumbles in the early weeks of the coronavirus crisis was inadequate testing. Thanks to a series of poor decisions by federal officials, the United States had far too little capacity to test for COVID-19 throughout the month of February, hampering our ability to contain the spread of the virus.
America is finally testing for coronavirus in significant volumes
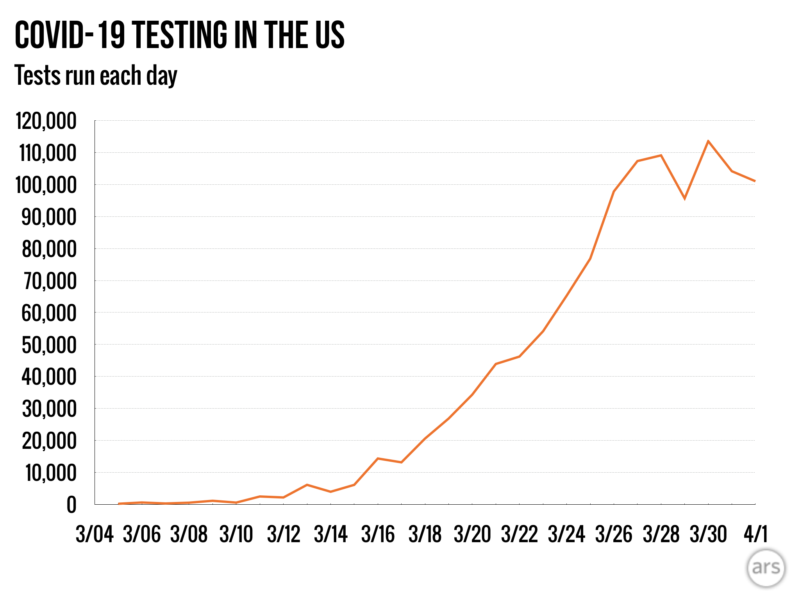
In early March, things seemed to be turning around. According to data from COVID Tracking Project, daily testing grew exponentially from a few hundred tests on March 5 to 107,000 tests last Friday, March 27.
But since then, progress has stalled. The US has been testing a bit over 100,000 people a day for the last six days—including 101,000 yesterday. And that's a cause for concern because the US will need to do considerably more testing to get its coronavirus outbreak under control.
Why testing matters
The most urgent need for testing is when a patient shows up at the hospital with coronavirus symptoms. Knowing if a patient actually has coronavirus or some other disease with similar symptoms determines what kinds of treatment are most appropriate. It also lets health care workers know whether they need to take precautions to avoid catching the coronavirus themselves.
Testing is also crucial for slowing the spread of coronavirus in the wider world. Ideally, when a patient is diagnosed with COVID-19, health officials would test everyone who has had close contact with that person. If someone else tested positive, officials would test all of their close contacts too. This process is known as contact tracing. Doing it on a wide-enough scale should allow officials to quickly identify and isolate almost everyone who has the disease.
You might not think that would matter now with so many people staying at home. But there are a fair number of people still working in essential industries who are at risk for catching COVID-19.
Amazon, for example, has had coronavirus cases at a growing number of fulfillment centers around the country. When these outbreaks occur, Amazon typically orders co-workers known to have had close contact to self-quarantine for 14 days. But those workers aren't necessarily tested. So if one of them passed COVID-19 on to someone else before their quarantine began, public officials wouldn't find out.
When to go back to work
So greater testing capacity would help improve treatment of patients and limit the spread of the coronavirus today. And it will become even more important once the current outbreak has peaked and public officials want to start sending people back to work.
If officials simply lifted quarantine restrictions without taking other precautions, the virus would resume its exponential growth and we'd wind up with a second large-scale outbreak. Aggressive contact tracing and quarantine policies are needed to make sure this doesn't happen. And that requires ample testing capacity.
Large-scale testing can also inform public officials' decision about when and how to lift restrictions. That's important because today's large-scale quarantine policy is having massive economic costs. The more data officials have about the spread of the coronavirus, the more precisely they can determine when and where it's safe to relax restrictions and the sooner they can let people go back to work.
Current testing levels aren’t enough
The countries that have been most successful at controlling their coronavirus outbreaks have done a lot more testing than the United States on a per capita basis.
America’s COVID-19 testing has stalled, and that’s a big problem
We'll need a lot more testing capacity to get the coronavirus under control.
Timothy B. Lee - 4/2/2020, 5:09 PM
One of America's biggest fumbles in the early weeks of the coronavirus crisis was inadequate testing. Thanks to a series of poor decisions by federal officials, the United States had far too little capacity to test for COVID-19 throughout the month of February, hampering our ability to contain the spread of the virus.
America is finally testing for coronavirus in significant volumes
In early March, things seemed to be turning around. According to data from COVID Tracking Project, daily testing grew exponentially from a few hundred tests on March 5 to 107,000 tests last Friday, March 27.
But since then, progress has stalled. The US has been testing a bit over 100,000 people a day for the last six days—including 101,000 yesterday. And that's a cause for concern because the US will need to do considerably more testing to get its coronavirus outbreak under control.
Why testing matters
The most urgent need for testing is when a patient shows up at the hospital with coronavirus symptoms. Knowing if a patient actually has coronavirus or some other disease with similar symptoms determines what kinds of treatment are most appropriate. It also lets health care workers know whether they need to take precautions to avoid catching the coronavirus themselves.
Testing is also crucial for slowing the spread of coronavirus in the wider world. Ideally, when a patient is diagnosed with COVID-19, health officials would test everyone who has had close contact with that person. If someone else tested positive, officials would test all of their close contacts too. This process is known as contact tracing. Doing it on a wide-enough scale should allow officials to quickly identify and isolate almost everyone who has the disease.
You might not think that would matter now with so many people staying at home. But there are a fair number of people still working in essential industries who are at risk for catching COVID-19.
Amazon, for example, has had coronavirus cases at a growing number of fulfillment centers around the country. When these outbreaks occur, Amazon typically orders co-workers known to have had close contact to self-quarantine for 14 days. But those workers aren't necessarily tested. So if one of them passed COVID-19 on to someone else before their quarantine began, public officials wouldn't find out.
When to go back to work
So greater testing capacity would help improve treatment of patients and limit the spread of the coronavirus today. And it will become even more important once the current outbreak has peaked and public officials want to start sending people back to work.
If officials simply lifted quarantine restrictions without taking other precautions, the virus would resume its exponential growth and we'd wind up with a second large-scale outbreak. Aggressive contact tracing and quarantine policies are needed to make sure this doesn't happen. And that requires ample testing capacity.
Large-scale testing can also inform public officials' decision about when and how to lift restrictions. That's important because today's large-scale quarantine policy is having massive economic costs. The more data officials have about the spread of the coronavirus, the more precisely they can determine when and where it's safe to relax restrictions and the sooner they can let people go back to work.
Current testing levels aren’t enough
The countries that have been most successful at controlling their coronavirus outbreaks have done a lot more testing than the United States on a per capita basis.
(continued in my first comment below)

Comments (5)
South Korea, for example, has performed 431,000 tests since its outbreak began. On a per capita basis, that's equivalent to 2.7 million tests in the US. We've only done 1.1 million tests so far, according to the COVID Tracking Project.
South Korea's testing has actually leveled off at around 10,000 tests per day. But that's because South Korea has gotten its coronavirus outbreak under control. It's had 9,976 total infections, and it had only 89 new infections on Thursday. In contrast, the US has had more than 236,000 infections, with tens of thousands of new infections daily. That's far more than South Korea even after you adjust for population. So we're going to need much more testing to get the situation under control.
Another example: Germany is conducting 50,000 tests per day. That's about twice as much testing as the US on a per capita basis. Germany's aggressive testing may have helped the country keep its coronavirus fatality rate low.
Governors in the United States say that a shortage of testing supplies is hampering their fight against the virus. The New York Times recently obtained audio of a call between governors and President Trump:
Gov. Steve Bullock of Montana, a Democrat, said that officials in his state were trying to do "contact tracing"—tracking down people who have come into contact with those who have tested positive—but that they were struggling because "we don’t have adequate tests."
"We have a desperate need for testing kits," Washington Gov. Jay Inslee told CNN on Sunday.
The rising rate of positive results is an ominous sign
When testing resources are scarce, health professionals prioritize testing people with obvious COVID-19 symptoms. If testing capacity were growing faster than coronavirus infections, we would expect more testing of people with milder symptoms or no symptoms at all. That should lead to a declining rate of positive test results.
Instead, the fraction of positive test results has been steadily rising over the last two weeks. The week of March 15, around 13 percent of coronavirus tests produced positive results, according to COVID Tracking Project data. Last week it was 17 percent. So far this week, 22 percent of coronavirus tests have produced positive results. Yesterday's figure was more than 25 percent.
This doesn't necessarily mean that the number of infections is growing faster than our testing capacity. For example, it's possible that as health care workers have become more familiar with the virus they've gotten better at identifying probable coronavirus cases, allowing them to prioritize testing of people who are likely to have the virus.
But it does suggest that our testing capacity isn't significantly outpacing the number of infections. And a 25 percent positive testing rate also suggests that we don't currently have enough testing capacity to truly bring the virus under control, because thorough contact tracing is going to require testing a lot more than four people for every infection.
New York is the hardest hit
So far we've looked at aggregated national data, which can mask regional variations. Luckily, the COVID Tracking Project also has state-by-state data, harvested from state websites. (The project's national numbers come from adding up these state figures.)
The situation in the hardest-hit states underscores the broader problem we've already discussed. Very high rates of positive test results suggest that states are focusing on testing patients with obvious COVID-19 symptoms, leaving few tests available for broader efforts to slow the spread of the virus.
By far the worst-hit region is the New York metropolitan area. New York state has 84,000 confirmed coronavirus, while neighboring New Jersey has another 22,000. These two states account for almost half of America's 236,000 coronavirus cases.
New York and New Jersey have suffered two of the highest coronavirus death rates in the US, both in absolute terms and on a per capita basis.
And these two states' testing situations are especially dire. New York has done 220,000 coronavirus tests. That's more than one test for every hundred New Yorkers, the highest per capita testing rate of any state. But the state's 84,000 positive results translates to a 37 percent positive rate. Similarly, New Jersey has performed 52,000 tests—well above average on a per capita basis. But its rate of positive tests was 42 percent—the second highest figure in the nation.
Michigan et al.
Michigan has the dubious distinction of the highest rate of positive coronavirus tests, at 44 percent. Michigan has more than 9,000 confirmed coronavirus cases and has had 337 coronavirus deaths—the third highest after New York and New Jersey. But unlike those states, Michigan has a below-average testing rate, with only about 0.2 tests per hundred people. Michigan desperately needs to test more.
Washington state was one of the first states to suffer a significant coronavirus outbreak. But thanks, perhaps, to aggressive responses by state officials, Washington has been relatively successful at containing the outbreak. The state has 5,600 confirmed coronavirus cases and has suffered 224 coronavirus deaths.
Those are fairly high numbers by national standards, but they are a relative improvement from a couple of weeks ago, when the Seattle area was seen as perhaps the nation's leading hot spot. Washington state has conducted an impressive 66,000 tests, with only 8.5 percent showing up as positive.
California has 8,200 confirmed cases. On a per-capita basis, that makes California about average among the states. However, that figure comes with a big caveat: California has only gotten results back for about 30,000 tests, and it says it has 57,400 test results pending. The tests returned so far have shown a positive rate of 27 percent. If the backlogged specimens are positive at a similar rate, it will add thousands of people to California's count of confirmed coronavirus carriers. That would put California among the top 10 states with the highest per capita coronavirus cases.
Labs are struggling to keep up with demand
It's not clear why the growth of testing has stalled out in the last week. On a basic level, the nation's testing laboratories probably just aren't set up to deal with sudden, massive spikes in demand. The dramatic differences in testing numbers from state to state also suggest a lack of national coordination to match health care facilities with the greatest need to labs with spare capacity.
A deeply reported piece in The Atlantic this week casts some light on America's testing predicament. It argues that private testing labs, which "now dominate the country's testing capacity" simply haven't been able to keep up with surging demand. "Testing backlogs have ballooned," Alexis Madrigal and Robinson Meyer write.
The writers report that Quest, one of the nation's two largest private testing companies along with LabCorp, has struggled to scale up its operations. Its primary testing lab is based in California, which might help explain why that state has such a backlog of pending tests.
A company spokeswoman told The Atlantic that its initial efforts in California simply hadn't been able to keep up with demand.
"There was a tremendous demand because we only had the one laboratory [in San Juan Capistrano] for about a week or more, and all the demand was being funneled into that laboratory," she told The Atlantic. But she claimed the company was catching up. "The average turnaround time nationally is four to five days, from the time where we collect the specimen to when we report the results out," she said—though she admitted that some results take "several days" longer.
More testing is vital for public health and the economy
Whatever problems are plaguing Quest and other testing labs, it's vitally important that they figure out how to dramatically increase their throughput. First and foremost, more testing will allow health care workers to more effectively treat patients while also keeping themselves safe. But more testing will also be crucial to minimizing the epidemic's impact on the US economy.
The extreme self-quarantine measures in place across the United States are vital to control the spread of the coronavirus, but they're also stupendously expensive in economic terms. On Thursday, we learned that 6.6 million people filed initial unemployment claims last week. That was double the figure from the previous week and 10 times higher than the previous weekly record, set during the Great Recession.
Every additional week that people are forced to stay at home costs the nation's economy tens of billions of dollars. Large-scale testing is going to be an essential part of any strategy for putting the nation back to work promptly while keeping the spread of coronavirus under control.
In recent weeks, the nation has seen a frantic effort to increase ventilator production to help deal with an expected surge of hospitalized coronavirus patients. Companies outside the medical-device industry—from GM and Ford to vacuum cleaner maker Dyson—have been looking for ways to help increase output.
We should feel the same sense of urgency to figure out how to increase the nation's coronavirus testing capacity. Because our current rate of testing—around 100,000 tests per day—isn't nearly enough.
My colleague John Timmer suggests one way this might happen. He points out that most universities have large capacity to conduct laboratory tests, but the infrastructure doesn't exist to get samples and supplies to people who can do the work. A better national system to coordinate testing efforts might be a big help here.
Sad but true...
The rest are either currently infected, or likely susceptible to being infected.
It might be noted, that a medical worker, who has recovered from Covid-19, would be highly valued to treat Covid-19 patients.